It was Friday, November 11 2016 and I was not feeling well, a bit flat, but I still went to work. I worked for the Government in Child Protection. At about 10am I told my bosses I was not feeling well and booked in to see a GP. I couldn’t get in to see my normal doctor, so I saw a duty doctor. My hands were aching so I thought I had Ross River, as I have had it before and my hands used to ache. The doctor ordered a blood test and said I probably had a virus and should go home and take it easy, which I did.
The next day I was going to drive to our family farm, but because I still felt unwell, I decided not to. My wife asked me to help her to pick up the family car from the local mechanics. As I walked out the front door I felt faint, so I returned to the couch and sat down. My wife phoned for an ambulance. I was taken to Mt Barker Hospital where they gave me an ECG and took a blood test. My wife said I was still conscious, but I cannot now remember. I was rushed to the RAH and upon arrival I was taken in for an angiogram. I had 2 stents placed into one artery and then I was taken to a ward.
Later that evening my blood pressure dropped and an ultrasound of my heart showed that my Mitral valve was damaged from my heart attack and could not be repaired. I was then taken down to Intensive Care and had an Intra-Aortic balloon pump inserted, via my groin, to stop the blood going back into my heart until they were able to insert a new valve. I made it through that night.
On Sunday November 13 I was taken in for an 8-hour surgery to replace my mitral valve with an artificial one, then taken back to ICU to be stabilised by the talented ICU nurses. I was in a critical condition and they told my wife in the next 12 to 18 hours they will know more. I had my family in the ICU waiting room and they didn’t want to leave. I was also put on dialysis at some stage.
I was in an induced coma for 8 days – Day 4, November 15 – tried to take me off sedation but I continued to cough. November 16 – wound drains removed and medication changed. November 17 – more heart medications stopped as some of the drugs were restricting blood vessels and some of my fingers and toes looked a bit dark. My wife thought they would be OK once the drugs were out my system. I was taken off oxygen to give my lungs some exercise.
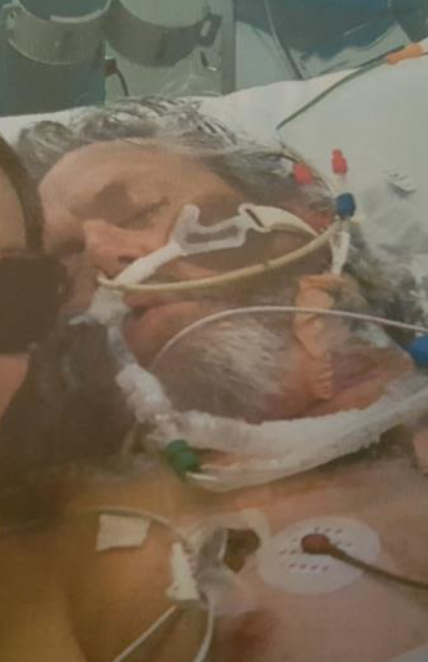
Sunday November 20 – The nurses changed my dressings on my hands and feet where I had some blisters. I was still on kidney dialysis and respirator. My wife had many photos printed of my family so all the nurses knew who every family member was. The nurse took me off sedation so everyone was waiting for me to wake. I had many friends and family members visit me even though I was out to it
Monday week 2 – My brother came in to see me and I started to waken. My eyes opened and I started to move my neck, head shoulder and legs. When I woke, I remembered having a bad dream and was so glad it wasn’t real, but at the time it felt so real. I had many dreams and there are 3 that I mainly remember. I was still in shock from the first dream and it took me quite a while to work out it wasn’t real, just a dream.

When I woke up properly, I could see my fingers and toes appeared to be black. I thought to myself, ‘well they are stuffed’. My fingers felt like burnt sausages and they were very stiff. My toes were also black and one third of both my feet. This didn’t worry me at the time because I was happy just to wake up. The nurses had given me a diary so anyone could write in it – family, friends, doctors, nurses etc.
I was told at some stage that I’d had 2 strokes and pneumonia. I remember asking a nurse why am I getting a CT scan and she said I had pneumonia. Communication is sometimes a problem between patient and/or family, and in some circumstances, people don’t want to know because it causes trauma. It did shock me at the time.
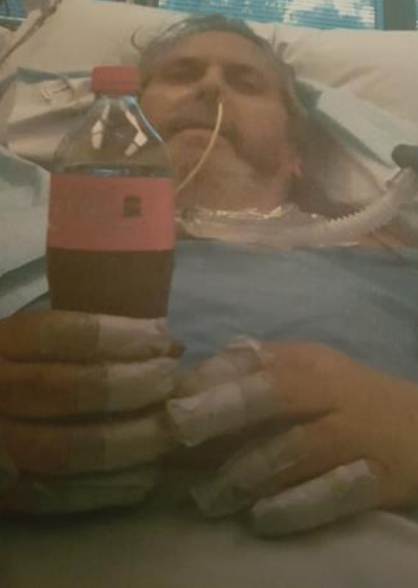
December 11, Day 30 – I was taken outside for the first time. By day 35, I was getting extremely frustrated that I couldn’t speak due to my tracheostomy. I remember having to use a white board to communicate, and for the nurses to write their names on for each shift.
December 25 – Christmas was great in ICU. They decorated my room and I had my family visit. On 29 December I was back in surgery to fix my chest so it would hold together. I was told I had an infection so my chest was still open; I didn’t want to look down at my chest at that stage.
Friday January 6 – It’s my birthday, I had friends and family visit all day. I also had a cardiac doctor come and see me and wish me all the best for the upcoming operation. Two days later my local GP visited me, but because I was on some heavy medication, I couldn’t remember the visit. The nurse said she had never seen a GP come in to see a patient before. On 9 January I had my local 2 Baptist church ministers, one retired, give Holy Communion because we were unsure if I would survive the operation the following day.
10 January, a big day. Another 4 – 5 hour operation to close my chest that had been open for nearly 2 weeks, and to have my fingers and all of my toes, including the front of my feet, amputated. One of the ICU nurses, Nihada,put her face nose to nose with my face and said with a big smile, ‘When you wake up, it will be my face you will see Chris’. This is what happened after the operation. Nihada was there and I very much appreciated her. If anyone knows Nihada, she is larger than life, with a compassionate personality. When I say large, I don’t mean in size, just her heart.

19 January – I finally had my tracheostomy removed and I was able to speak without using a white board. I also had my first shower since being admitted to hospital. The nurses let me play the rock & roll music I liked in my room and when I had my shower.
On January 24 Dr Hugh Cullen said to me he does 230 heart operations a year, and only 2 people out of that have had what has happened to me. I don’t know how many survived out of the 2! During this whole time, I only had one nurse that worried me, so I complained to Svatka, who quickly fixed the problem. The nurse was an agency fill in, but she made me worried all night. All the nurses were 5 star and I can’t say enough how fantastic they were. At some stage, I had an infection which they think contributed to me being delusional; I was asking how do I get out of here and calling a friend’s name out.
February 12 – They were trying to encourage me that going to a ward was a great step forward but I wasn’t convinced. I loved all the nurses, and had a great rapport with them. I was finally moved to a ward and had a lot of physio with Rocky… I love that name. I couldn’t walk from being in bed for so long… I also had to have a crane lifter to get me out of bed.
I eventually got moved to the Repat Hospital for rehabilitation, and then developed a blood infection and ended up back in the Royal Adelaide Hospital. I did recover and they moved me back to the Repat. The level of care was nothing like the RAH, and many times I wet myself because no one came when I pressed the buzzer. This was distressing for me but it didn’t appear to worry the nurses. The rehabilitation was extremely hard and I wondered if I would ever walk again. I hated ‘sit to stands’. I used a walker for months, then went to a walking stick. I couldn’t believe I actually had to learn to walk again and didn’t realise what I took for granted could be so hard.
Things I thought about – I had to come to terms with the fact that my working life was over. I would find it hard to use a computer and I could only stand for a short time because of my feet. I also did a lot of driving, and now having a disability, this was going to be a game changer, especially driving with young children in the car. I loved my job working in Child Protection. I had been doing this job for 25 years. One of the hardest things was I was not going to achieve my work goals and I have felt down about that for many years since my heart attack.
The Repat wouldn’t let me go home without support… support … What’s this about? I thought I would just go home. The Repat let me have some day visits for a few hours. They also requested I have a carer for 24 hours a week. It was a time when it was changing to NDIS. I was approved but they couldn’t find any carers in the Adelaide Hills. They eventually found some and I was able to go home, this was after 7 months of me being in hospital. When I returned home, I had frozen shoulders and couldn’t even move them, even going to the toilet… carers had to help me. I found this difficult to accept, especially for a man who has always been so independent. I went and saw a physio and after many visits, fixed my shoulders.

My kidney function had dropped to around 10 percent, but I was still not on dialysis. It was just one more thing to worry about after what I had been through. I received a letter in the post to hand in my driver’s licence as they said I would not be able to drive for 12 months because of my 2 strokes. I didn’t care at the time. I was still struggling to walk and didn’t know how I would go with no fingers. Financially I had used up all my Sick Leave and Long Service Leave. I had to think about what I was going to do in the future. I was told my superannuation will have medical insurance for death or disablement, so I looked into it and put in a claim that was accepted. I had to resign my position at work. My work colleagues gave me a big send-off event.

It has been an enormous change for me. I used to help people in my field of work, and in my own time, and now have to accept help from others. That has been an extremely hard thing for me to accept. Over time, I learnt to walk unaided. I still can’t use my right hand very well; it folded inwards after my fingers were amputated. I have waited 4 years for an operation to straighten my right hand out.
A year after I handed in my driver’s licence, I decided I wanted to get it back. I had to find out how?, when? etc. I eventually found out the steps; go to my doctor, then go to Flinders Fitness Assessment Clinic at Flinders Medical Centre for a driving test. I did an eye test and then went back at a later date for a driving test. I was very good, but the OT in the back seat must have had a bad night and didn’t pass me. I then was booked in for the next month and had no problem getting my licence back.
I have found that some people treat you like a cripple and can be rude and obnoxious. I guess I am now somewhat having a disability. NDIS has been great, but it can be confusing at first; they know how to make things complicated. I like the KIS method… ‘Keep it simple’. To have a disability, this is one of the best countries in the world who truly look after people with a disability. I have no complaints because when I left the hospital, I thought I would be on my own without any support.
I did see a psychologist for a while because I was grieving the loss of being independent; I couldn’t drive a car or ride my motorcycle, put on my clothes and do up my buttons, I couldn’t eat food I liked because of my kidneys. I had to give up the job I loved. I had to now get used to doing nothing. The list goes on and on, and I was extremely angry inside. This is part of the grieving process… coming to terms that you will not be able to do things like you used to. I did the ‘Why me’? I normally goal set then go for it, but I’m still looking for direction at the moment. I am just an ordinary human being that now has to have different realistic expectations.
One positive is that I have not had depression. In 2006 I had an accident, resulting in me getting depression, so I know what it is. Yes, I have been down, like all of us, but depression is far deeper. I have been close at times and have bounced on the top of depression. People that have never had it wouldn’t understand, so I can say now I was glad to have had it, but would never want it again. I now focus on what I can still do, not what I have lost. Easier said than done some days, it is what it is. I still have two great carers doing 24 hours a week who look after me. There is much more to my story than I have not written here.
Chris

This story first appeared in the Survive and Thrive Newsletter #4 February 2021. We thank Chris for giving us permission to share this story on the My Life After ICU website.